Navigating Inflammation and Pain
Your compass to finishing the healing cycle and resolving inflammation.

In the realm of middle age and retirement, life weaves experiences like memories, yet it also brings forth occasional groans when rising from a chair. Remember when bending to pick up something wasn't a mental pep talk?
Pain, a universal experience, evolves, growing more prevalent as we journey from midlife to retirement. For those in middle age and the retirement phase, pain isn't occasional; it can become a companion impacting our quality of life.
As our bodies progress through these stages, wear and tear on joints, muscles, and bones can lead to persistent pain. Simple tasks become challenges, and chronic pain can affect emotions, sleep, and social interactions, dimming the retirement glow.
Amid life's chapters, our bodies face challenges from nicks to injuries. Inflammation, crucial to healing, sometimes falters, causing enduring discomfort and chronic pain. In this article, we'll explore the world of inflammation, uncover the healing cycle's role, and see how an incomplete cycle can cast shadows on our lives.
The Multifaceted World of "Ouch"
From the spontaneous "why did I think I could do that again?" moments to the daily reminders of aging, pain and inflammation are interlinked.
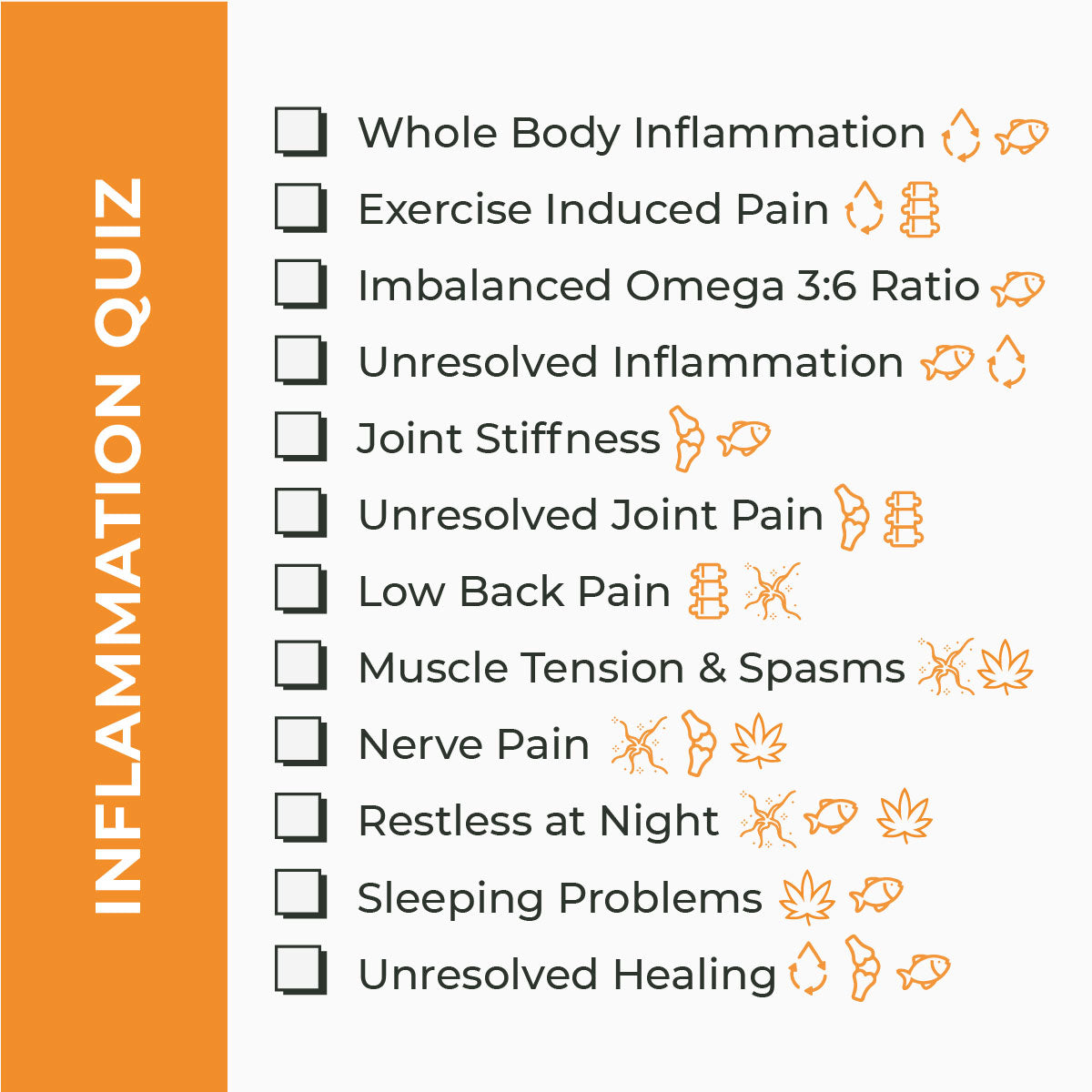
While pain is a symptom, inflammation is often the underlying cause. Here's a breakdown:
- Acute Pain & Inflammation: Often results from injuries, infections, or surgeries. It's a short-term response, usually localized, like a sprained ankle or a surgical incision.
- Chronic Pain & Inflammation: Persists beyond the typical healing time. Conditions like osteoarthritis, where joint cartilage degrades over time, lead to chronic inflammation and pain.
Body parts commonly affected include:
- Joints: Especially knees, hips, and hands, often due to arthritis.
- Back: Resulting from issues like herniated discs or spinal stenosis.
- Muscles: From conditions like fibromyalgia or long-term muscle strain.
- Nerves: Conditions like diabetic neuropathy or post-herpetic neuralgia can cause nerve pain.
Inflammation Resolution: The Key to Addressing Chronic Pain
Inflammation is the body's natural response to injury or infection. However, when inflammation becomes chronic, it can result in ongoing pain. The resolution of inflammation is crucial in addressing and potentially alleviating this pain. By targeting the root cause, the inflammatory response, rather than just the symptom (pain), we can achieve more effective and lasting relief.
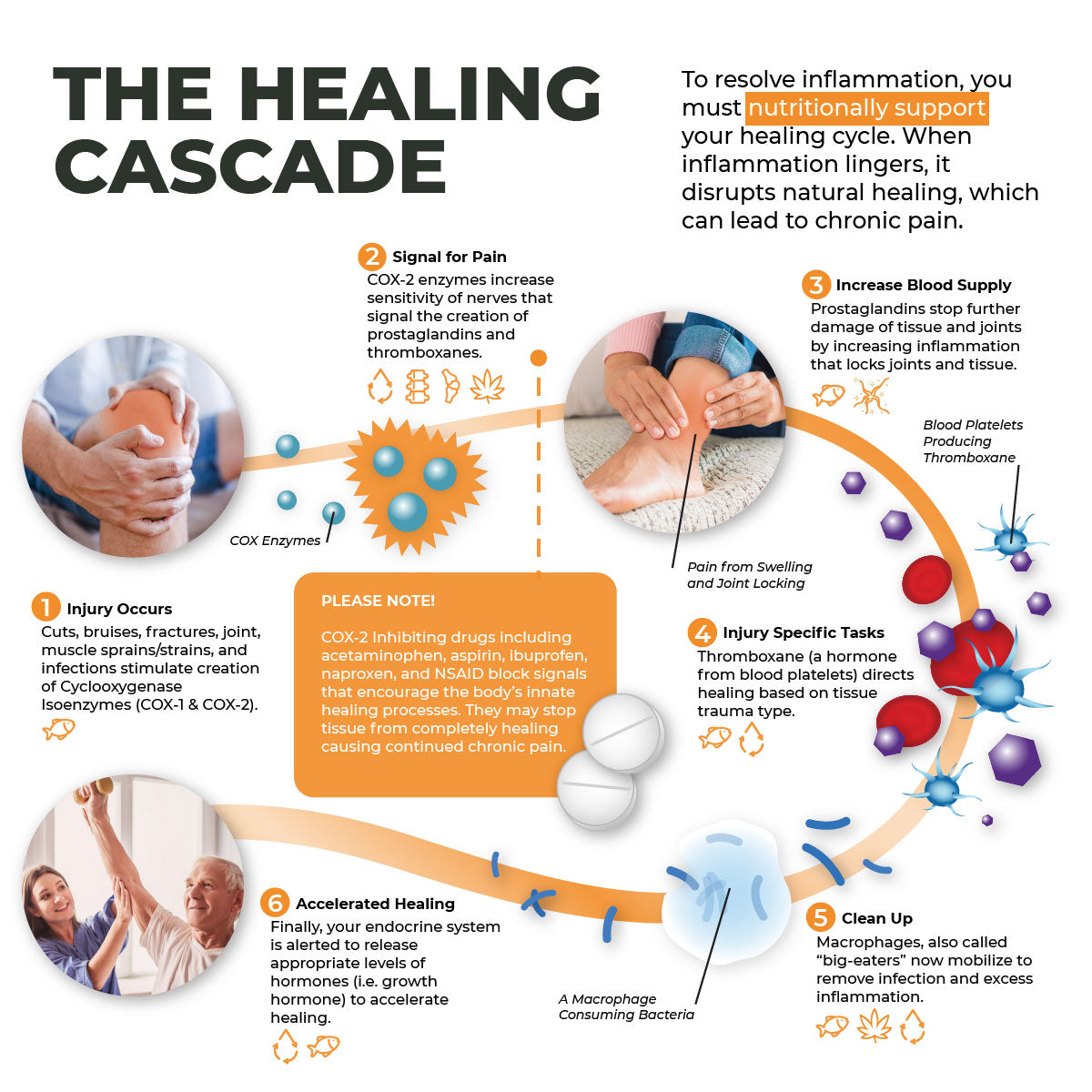
The Healing Cascade: A Natural Symphony
Imagine your body as a finely tuned orchestra, with each instrument playing its unique part to produce a harmonious melody of healing. When injury strikes, our body's first responders, like COX-2 enzymes, orchestrate the pain and inflammation signals that are vital for repair.
Prostaglandins step in to increase blood supply, preventing further damage while locking joints and tissues to safeguard them. This initial response is crucial to setting the stage for the healing process.
Enter Macrophages: The Cleanup Crew
As the healing symphony continues, macrophages step in as the diligent cleanup crew. Aptly named "big-eaters," they remove infections and excess inflammation, paving the way for the next act of healing.
This meticulous cleanup ensures that the stage is set for accelerated healing, with the endocrine system releasing hormones like growth hormone to speed up recovery.
The Puzzle of Chronic Pain: Incomplete Healing
However, for many individuals, the healing symphony can hit a sour note. Chronic pain, a persistent and unwelcome companion, can result from an incomplete healing cycle. This is where the narrative takes a turn.
Unresolved inflammation arises when the healing process is disrupted, leaving our body in a state of limbo. Factors such as dietary imbalances, specific pain medications, lifestyle choices, infections, and underlying health conditions can contribute to this incomplete cycle.


Research-Backed Solutions: Mediherb and Standard Process Products
Boswellia Complex by Mediherb: A standout product backed by research, this complex offers significant benefits. After just 4 weeks, users reported a 25% decrease in WOMAC Index scores, indicating reductions in pain, stiffness, and improved physical function. Key ingredients include Boswellia, Celery Seed, Ginger, and Turmeric. It not only supports healthy circulation but also aids in maintaining a healthy GI inflammatory response.
Turmeric Forte by Mediherb: Turmeric has been recognized for its anti-inflammatory properties for centuries. This specific formulation, combined with fenugreek seed fiber extract, ensures prolonged retention in the body. It's absorption rate is impressively higher than curcumin alone (24.8x higher), and its relief lasts up to five times longer. Notably, it supports the resolution phase of inflammation.
Ligaplex II by Standard Process: Designed specifically for connective tissue and joint support, this supplement maintains the health of connective tissues and provides essential nutrients for the skeletal system. It's an amalgamation of ingredients from products known to benefit skeletal health, making it an excellent choice for older adults.
Cod Liver Oil by Standard Process: A standout product backed by research, this omega-3 supplement offers significant benefits. It's known to support healthy inflammatory pathways, which is crucial for managing chronic pain.


Consistency is Vital to Inflammation Resolution
For natural supplements to be effective, consistency is crucial. Establishing a routine ensures that the body receives a steady supply of beneficial compounds. An autoship program guarantees that you never run out of your supplements, ensuring uninterrupted support for pain and inflammation management.
- Boswellia Complex: 3 tablets a day, best taken every 6 hours for healthy patients. Optimal with high-fat meals or alongside fish oil.
- Turmeric Forte: 3 tablets a day, but some people consume 6/day (divided doses) for the first bottle… remember it's contraindicated with blood thinners, talk to your doctor about options.
- Ligaplex II: 2 tablets, 3 times a day. We suggest one 90-day cycle and then reassess.
- Cod Liver Oil: 1 peral twice a day. These large perles are not for everyone, if you have problems swallowing large pills, then we recommend Tuna Omega Oil or Chewable Tuna Oil (which kids like). Once again fish oils thin the blood and are contraindicated with blood thinners.


The Importance of Fish Oils and Anti-Inflammation Diet
Diet plays a significant role in managing inflammation. Incorporate omega-3 rich foods like fish, flaxseeds, and walnuts. Prioritize fruits and vegetables, especially berries, tomatoes, and leafy greens. Limit processed foods, refined sugars, and excessive red meat. Hydration is key, so drink plenty of water.
Fish oils, rich in omega-3 fatty acids like EPA and DHA, are renowned for their potential anti-inflammatory properties, which may help alleviate pain and inflammation. They can generate anti-inflammatory eicosanoids, counteracting the pro-inflammatory ones and inhibit pivotal inflammatory pathways, thus decreasing the production of inflammation-promoting chemicals.
These fatty acids also aid in resolving inflammation by preventing the influx of inflammatory cells and facilitating their clearance from inflammation sites. The reduction in inflammation can also ease pain, especially in conditions like arthritis. Furthermore, DHA enhances cell membrane health in the nervous system, possibly mitigating inflammation and refining pain signaling.
In conclusion, understanding pain and its root causes is crucial for effective management, especially for older individuals. Natural, research-backed solutions like those from Mediherb and Standard Process offer promising avenues for relief, especially when paired with a balanced, anti-inflammatory diet. Always consult with a healthcare professional before starting any new supplement or dietary changes.

Helpful links and references
1. Kumar D, Jacob D, Subhash PS et al. J Funct Foods 2016; 22, 578-587
2. Firestein, G. S. (2003). Evolving concepts of rheumatoid arthritis. Nature, 423(6937), 356–361.
3. Serhan, C. N., Brain, S. D., Buckley, C. D., Gilroy, D. W., Haslett, C., O'Neill, L. A. J., Perretti, M., Rossi, A. G., & Wallace, J. L. (2007). Resolution of inflammation: state of the art, definitions and terms. FASEB Journal, 21(2), 325–332.
4. Gioxari, A., Kaliora, A. C., Marantidou, F., & Panagiotakos, D. P. (2018). Intake of ω-3 polyunsaturated fatty acids in patients with rheumatoid arthritis: A systematic review and meta-analysis. Nutrition, 45, 114–124.e4.
5. Aggarwal, B. B., & Harikumar, K. B. (2009). Potential therapeutic effects of curcumin, the anti-inflammatory agent, against neurodegenerative, cardiovascular, pulmonary, metabolic, autoimmune and neoplastic diseases. The International Journal of Biochemistry & Cell Biology, 41(1), 40–59.
6. Calder, P. C. (2006). n−3 Polyunsaturated fatty acids, inflammation, and inflammatory diseases. The American Journal of Clinical Nutrition, 83(6 Suppl), 1505S-1519S.
7. Ricciotti, E., & FitzGerald, G. A. (2011). Prostaglandins and Inflammation. Arteriosclerosis, Thrombosis, and Vascular Biology, 31(5), 986–1000.
8. Wynn, T. A., & Vannella, K. M. (2016). Macrophages in Tissue Repair, Regeneration, and Fibrosis. Immunity, 44(3), 450–462.
9. Medzhitov, R. (2008). Origin and physiological roles of inflammation. Nature, 454(7203), 428–435.
10. Molton, I. R., & Terrill, A. L. (2014). Overview of persistent pain in older adults. American Psychologist, 69(2), 197–207.
